Category
- Best Peptides for muscle growth
- Geno Pharma Domestic Warehouse 2 (Canada&USA)
- GPH(Domestic Shipping US) Warehouse 1
- Human Pharma Premium
- Phar Labs Premium-Select
- Steroids on Sale USA, Real Steroids Online
- New arrivals in USA
- Most popular steroids in USA
- Antiestrogens / Gonadotropins
- Bangkok Steroid USA
- Biopharma Steroid USA
- British Dragon
- Anabolic Steroids for Horses
- Fat-burners
- Gen Pharma USA
- Medical Pharma Steroid USA
- Medical Tech Steroid USA
- Novocrine Steroids
- HGH USA
- Omega Labs Steroid USA
- Rotterdam Steroids USA
- SARMs USA
- Sciroxx
- Sydgroup Steroid USA
- Big vetenary Steroid USA
- Watson Steroids
- XT Labs Steroids
Most Popular steroids USA
-
 Trenbolone 200 20ml - Sydgroup
$53.00
Trenbolone 200 20ml - Sydgroup
$53.00 -
 Primobolan for sale 100mg 10 ml Human Pharma in USA
$115.00
Primobolan for sale 100mg 10 ml Human Pharma in USA
$115.00 -
 NPP Steroid 100mg 10 ml Premium Domestic USA
NPP Steroid 100mg 10 ml Premium Domestic USA
$99.00Original price was: $99.00.$80.00Current price is: $80.00. -
 Anavar for Sale in USA – 10mg 80 Tabs GPH-Premium
Anavar for Sale in USA – 10mg 80 Tabs GPH-Premium
$110.00Original price was: $110.00.$80.00Current price is: $80.00. -
 Buy Anavar 10mg – Purchase Geno Pharma
$99.00
Buy Anavar 10mg – Purchase Geno Pharma
$99.00 -
 Testosterone Cypionate Buy 300mg 10ml Geno Pharma
$99.00
Testosterone Cypionate Buy 300mg 10ml Geno Pharma
$99.00 -
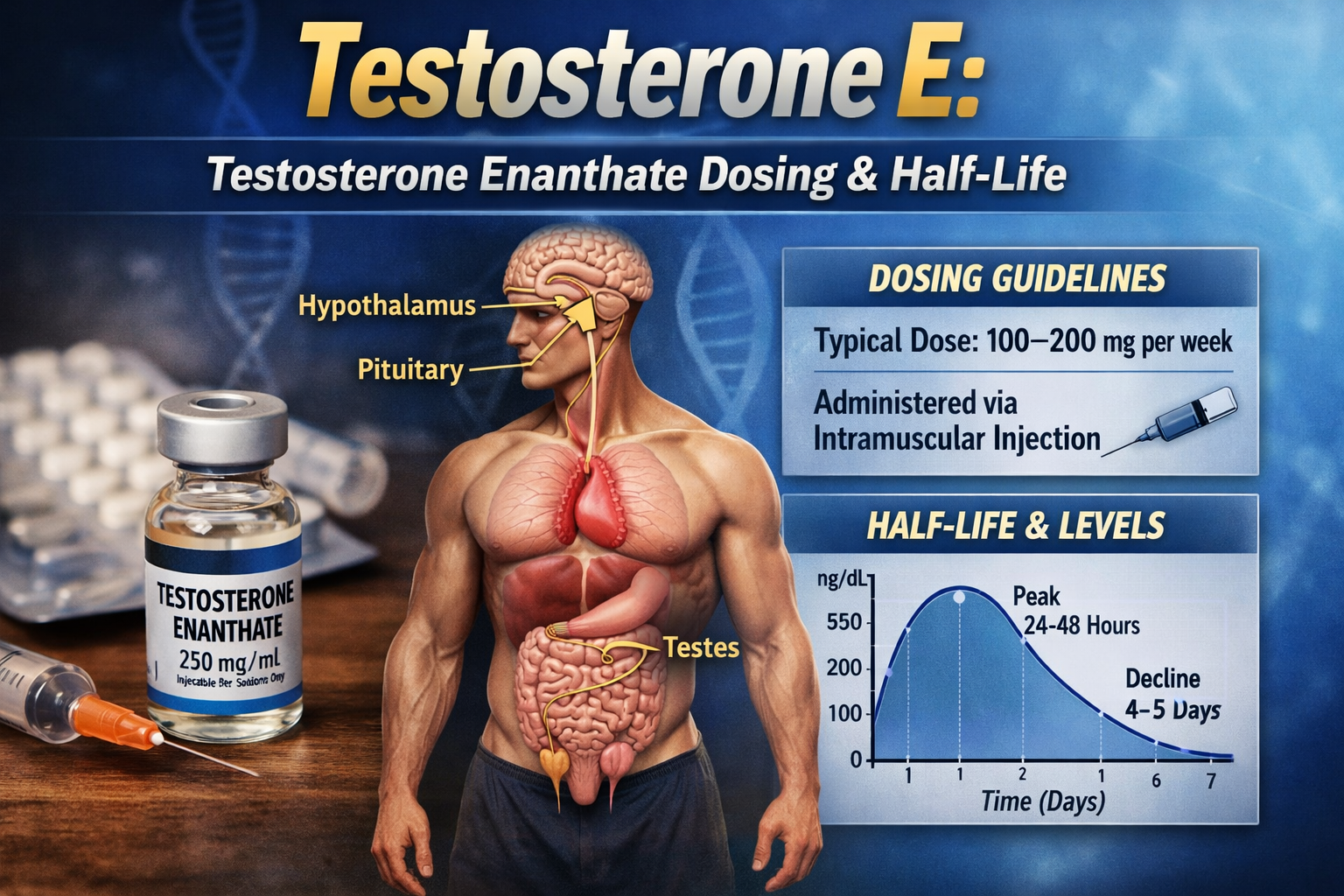
 Buy Testosterone E 300mg 10 ml Geno Pharma Domestic USA/CA
$99.00
Buy Testosterone E 300mg 10 ml Geno Pharma Domestic USA/CA
$99.00 -
 Testosterone Cypionate 200 Biopharma 10 amp
Testosterone Cypionate 200 Biopharma 10 amp
$99.00Original price was: $99.00.$72.00Current price is: $72.00. -
 Testosterone 400 Biopharma 10 Ampoules
Testosterone 400 Biopharma 10 Ampoules
$99.00Original price was: $99.00.$75.00Current price is: $75.00. -
 Eq 300 steroid Rotterdam 10ml
Eq 300 steroid Rotterdam 10ml
$79.00Original price was: $79.00.$69.00Current price is: $69.00. -
 Steroid Deca Geno Pharma 300mg 10ml
Steroid Deca Geno Pharma 300mg 10ml
$110.00Original price was: $110.00.$99.00Current price is: $99.00. -
 Boldenone Cypionate 200 mg / 10 mL Geno Pharma
Boldenone Cypionate 200 mg / 10 mL Geno Pharma
$90.00Original price was: $90.00.$85.00Current price is: $85.00.

Redotex 30 capsules Buy Steroids Online
$77.00
Each CAPSULE contains:
D-Norpseudoephedrine Hydrochloride 50.00 mg
Aloin 16.20 mg
Atropine sulfate 0.36 mg
Diazepam 8.00mg
Triiodothyronine Sodium equivalent to 0.075 mg of Triiodothyronine
Excipient cbp 1 capsule
THERAPEUTIC INDICATIONS: Anorexigenic.
Out of stock
Share this page:
- Share on X (Opens in new window) X
- Share on Facebook (Opens in new window) Facebook
- Email a link to a friend (Opens in new window) Email
- Share on LinkedIn (Opens in new window) LinkedIn
- Share on Reddit (Opens in new window) Reddit
- Share on Pinterest (Opens in new window) Pinterest
- Share on Telegram (Opens in new window) Telegram
- Share on WhatsApp (Opens in new window) WhatsApp
- Share on Tumblr (Opens in new window) Tumblr
Redotex 30 capsules Buy Steroids Online
Auxiliary in the treatment of exogenous obesity.
Obesity is the most important nutritional disorder worldwide with serious adverse effects on health, associated with an increase in morbidity and mortality, in such a way that weight loss allows to significantly reduce these risks. A small weight loss is accompanied by significant improvements in blood pressure; glucose tolerance and serum lipid concentration. Thus, the usefulness of pharmacotherapy for weight loss should not be underestimated. Thus, treatment is indicated when the risks of obesity outweigh the risks associated with any type of treatment. Due to the distinctive characteristic of obesity, as a chronic disease that is difficult to treat, but finally controllable. It is very important to consider that an effective treatment may involve more than one drug.
PHARMACOKINETICS AND PHARMACODYNAMICS: The pharmacodynamics of REDOTEX® corresponds to the synergistic action of its individual components, which results in a complementary therapeutic activity with good results.
The pharmacokinetics of REDOTEX® is the result of the balance and synergy of its individual components, without modifications because there is no interference between them. The combination of medications with different modes of action is an effective clinical strategy for the management of chronic diseases that are difficult to control, such as arterial hypertension and diabetes mellitus, a condition that also occurs with the treatment of obesity, especially since weight body is controlled by multiple factors that affect both calorie intake and energy loss.
The formulation of REDOTEX® in prolonged release capsules (Dialicels® technology), allows to maintain a prolonged and sustained release of the active ingredients of the drug, which modifies the maximum time (T max) and maintains a maximum concentration (C max) without peaks or troughs for a maximum of 12 hours after administration. The Dialicels® system helps to maintain the concentration of the drug in the tissues at optimal therapeutic levels throughout the treatment period, which means that the frequency of drug administration is reduced and, with it, the occurrence and intensity of undesirable effects is also reduced eliminate variability in its serum concentration, outside the therapeutic window.
Pharmacokinetics:
D-Norpseudoephedrine: It is almost completely and rapidly absorbed from the gastrointestinal tract, reaching a maximum concentration 1-2 hours after administration and with a variable half-life (from 3 to 10 hours) due to individual variations in absorption and/or elimination. It is evenly distributed to all tissues, crosses the blood-brain and placental barriers, and is found in breast milk. Between 55% and 75% of the dose is eliminated unchanged in the urine, the remainder is inactivated in the liver by n-methylation, parahydroxylation, and oxidative deamination.
Elimination through urine is variable and pH dependent, since it increases with acidification and decreases with alkalinization (half-life: pH 5 = 4 hrs-pH 8 = 13 hours), in such a way that about 40% of the administered dose is eliminated unchanged in the urine within 6 hours, and 87% to 96% of the drug is eliminated from the body within 24 hours.
L-Triiodothyronine (LT3): It is also absorbed in the digestive tract (95% in 4 hours). It binds to plasma proteins, being rapidly available for its activity in the tissues (Vmax. = 4 hours), its maximum activity is reached after 2 or 3 days (Cmax.).
Atropine sulfate: It is rapidly and completely absorbed from the gastrointestinal tract. It has a half-life of 2 hours and is eliminated almost completely and unchanged in the urine within 12 hours.
Aloin: Aloin is found in aloe, it shares a modified tricyclic anthracene nucleus with hydroxyl, methyl or carboxyl groups to form monoanthrones with laxative action. It acts in the intestinal lumen without absorption.
Diazepam: It is rapidly and completely absorbed through the intestinal mucosa. The maximum concentration peak is reached between 30 and 90 minutes (Cmax) after its administration. It is a long-acting agent with a half-life greater than 24 hours. It is 99% bound to plasma proteins and due to its high lipid solubility, it rapidly concentrates brain tissue such that its concentration in CSF is practically equal to that of free drug in plasma. It crosses the placental barrier and is secreted through breast milk. It is primarily metabolized in the liver by the cytochrome P450 family, in particular CYP3A4 and CYP2C19.
Its metabolism includes the formation of an N-dealkylated compound, nordazepam, with biological activity, which in turn undergoes hydroxylation in position 3, which gives rise to the synthesis of oxazepam to finally be conjugated with glucuronic acid, originating inactive compounds.
Cimetidine and oral contraceptives inhibit the N-dealkylation and 3-hydroxylation of benzodiazepines. Its most focused therapeutic application due to its prolonged half-life is anxiolytic. In the administration of the drug for a long time, the most important concept is elimination, since diazepam is mainly eliminated by the kidneys (70%). The microspheres of the Dialicels® prolonged-release capsules allow a sustained and prolonged release, do not cause interference between the drugs that are absorbed, and are also calculated not to produce accumulation or toxic levels. Patients who have received low doses of benzodiazepines for years do not usually experience adverse effects.
Pharmacodynamics:
D-Norpseudoephedrine:
Origin and chemistry: It is a derivative of Catha edulis and is the stereo-optical D-isomer of the 4 possible ephedrine. It has a light psychostimulant action, since it reduces feelings of fatigue and hunger. It has sympathomimetic properties, however, its adrenergic potency is 1,000 times less than ephedrine, which attenuates the possibility of increased blood pressure and heart rate. It is presented as a salt in the form of hydrochloride for pharmacological use.
Mechanism of action: D-Norpseudoephedrine produces a brief and slight release of catecholamines, of short duration and is associated with a rapid and temporary depletion phenomenon, acting at the level of easy release stores, with indirect action on both alpha and beta adrenergic receptors, with a preferential degree over beta adrenergic receptors.
At therapeutic doses, it does not stimulate the CNS, since its activity is located mainly in the hypothalamus, regulating the centers of satiety and appetite, which are very sensitive to adrenergic stimulation. In adipose tissue, the adrenergic stimulation caused by D-Norpseudoephedrine has a thermogenic and lipolytic effect. The central excitatory properties of D-Norpseudoephedrine do not produce the typical effects of ephedrine such as bronchoconstriction and arterial hypertension.
Pharmacological activity by devices and systems: The pharmacological profile of D-Norpseudoephedrine corresponds to that of adrenergic drugs that act indirectly, by releasing catecholamines. Next, the pharmacological profile for adrenergic drugs is described in a general way, considering that certain effects do not appear when they are used at the usual therapeutic doses.
CNS: Anorexigenic with central action on the appetite and satiety regulation centers located in the hypothalamus.
Cardiovascular: Shares the properties of indirect action adrenergics by releasing catecholamines. However, at the usual therapeutic doses, the effects of cardiac stimulation, tachycardia and arterial hypertension are observed to be attenuated.
Respiratory: By activating Beta receptors in the respiratory tract, it can induce a certain degree of bronchodilation.
Gastrointestinal: Decreases motility due to decreased tone, due to smooth muscle relaxation.
Uterine smooth muscle: Decreases motility and muscle tone, being more evident in the gravid uterus and especially during the last trimester of pregnancy.
Urinary Tract: Relaxes the detrusor muscle by contracting the trigone and the bladder sphincter, being able to induce urinary retention.
Metabolic Effects: Energy metabolism and thermogenesis may increase, reflecting in an increase in oxygen consumption.
Sense organs: It can cause mydriasis.
Clinical Pharmacology: The desirable effects of D-Norpseudoephedrine are its anorexigenic and thermogenic activity, which occur at doses that do not produce central side effects such as insomnia, hyperactivity, nervousness, or peripheral side effects such as tachycardia, hypertension, smooth muscle relaxation, urinary retention etc In patients under medical control and at recommended therapeutic doses, tolerance to its effects is not induced, so that the phenomenon of drug dependence or abuse is unlikely.
On the other hand, in patients with serious psychiatric problems or personality disorders, the therapeutic indication for the use of the drug is not justified. This same recommendation is also extended to those patients who also have neurological problems, eye problems such as glaucoma, cardiovascular, liver, kidney and urinary problems. Although no reports of teratogenicity or mutagenesis have been published, the drug is not recommended for the treatment of women during pregnancy or lactation.
Origin and chemistry: It is the monosodium salt of L-triiodothyronine, it is not a product of the endocrine gland. Considering the certainty of chemical purity, the administration of other molecules that are also present in the thyroid, such as calcitonin, is avoided. In this way, when obtained synthetically, it is a synthetic compound, with bioequivalent activity to endogenous thyroid hormone, which influences all tissues of the body and participates in the development and growth of the structure and functions of the CNS.
Mechanism of action: It acts at the level of the physiological receptors of the thyroid hormone, activating the nuclear transcription of a large number of genes with the result of a generalized increase in the functional activity of the entire organism; oxygen consumption in all tissues and basal metabolism and carbohydrates, lipids and proteins.
In addition, it promotes the expression of uncoupling protein 3 (UCP3), which increases thermogenesis since it favors the uncoupling of energy in the skeletal muscle mitochondria with a 15% increase in basal energy expenditure, which translates into a greater consumption desirable fat metabolism for the obese patient.
Thermogenesis increases 200% after the administration of norepinephrine or T3 separately, but increases 2000% when the two compounds are combined (as in the case of REDOTEX® D-Norpseudoephedrine as a sympathomimetic and Liothyronine as a basal metabolism accelerator). UCP3 expression is increased 5-fold after 5 days of T3 treatment. In obese subjects, the hypocaloric diet causes a decreased conversion of T4 to T3. On the other hand, thyroid hormones increase the number of β adrenergic receptors and thus increase the lipolytic effect of catecholamines, with a 16% increase in lipolytic activity.
Pharmacological activity by devices and systems: T3 is the quintessential representative of thermogenics. In the early 20th century, it was suggested that the obese have a “low metabolic rate.” In 1961, Goldberg suggested the possibility of euthyroid hypometabolism, thus justifying the use of T3 in obese patients, and thus Gordon named it metabolic obesity, based on the improved response to epinephrine after thyroid therapy.
In addition, T3 increases contractility and cardiac output, decreases peripheral resistance, increases depth of respiration, gastrointestinal motility, reflex speed, and tissue flow due to vasodilation. T3 also corrects hypothermia by increasing basal metabolism. Clinical studies have shown that a 320/kcal per day diet to which 25 μg of T3 was added three times a day, increased weight loss by 32%, while nitrogen balance did not change.
In a 10-week randomized, placebo-controlled, crossover study, 16 patients received T3 1000 kcal/day and 75 μg three times daily for 4 weeks. During treatment, the serum concentration more than doubled; weight change in the placebo group was +3.2 kg, and for those receiving T3 it was -3.9 kg; heart rate increased on average from 79 to 86 beats per minute (8.2%). In addition, high weight increases the production of leptin and this in turn stimulates the production of TSH, so it is very important to compensate for the decrease in TSH, and therefore in T3, that occurs in the patient during weight loss with the therapeutic purpose of stimulating energy expenditure.
The goal of caloric restriction is to maximize fat loss and minimize protein loss, Burman (1979) and Wilson (1981) found no increase in nitrogen excretion using low doses of T3. Which translates the safety of the use of T3 without producing protein catabolism.
Clinical Pharmacology: Its indications refer to the nosology associated with a relative deficiency of thyroid hormone. Its use is contraindicated in patients with thyrotoxicosis and adrenal insufficiency. It should be used with great care in patients with cardiovascular problems, the risk increases with age.
Atropine:
Origin and chemistry: Atropine (d,l-hyoscyamine), a natural muscarinic receptor antagonist, is an alkaloid found in plants of the belladonna group (family Solanaceae). It is found on Datura stramonium and Jamestown grass. It is an organic ester formed from the combination of an aromatic acid, the tropic acid, and complex organic bases, such as tropine or scopine. It occurs in the form of sulfate.
Mechanism of action: Atropine acts by competing for the muscarinic receptors M1 and M2 with the neurotransmitter acetylcholine, both in the CNS and in the peripheral. This property causes its effects to be present in the brain and in all the organs innervated by the parasympathetic ANS. At average clinical doses of 0.4 to 0.6 mg. HR decreases 4 to 8 beats per minute.
Atropine can completely abolish the copious parasympathetically induced aqueous secretion and inhibits sweat gland activity, making the skin hot and dry.
Pharmacological activity by devices and systems: Atropine presents the reference pharmacological profile of antimuscarinic activity. The intensity of its effects is dose dependent. Choline esters and anticholinesterase agents can antagonize the effects of atropine by displacing it from the muscarinic cholinergic receptor, being the antidotes of choice.
CNS: At therapeutic doses (0.5 to 1 mg), it produces a slight vagal excitation as a result of stimulation of the medulla oblongata and various brain centers.
Cardiovascular: At therapeutic doses there is no effect on blood pressure and at doses of 0.4 to 0.6 mg it decreases heart rate.
Respiratory: Respiratory tract secretions are inhibited and bronchodilation occurs.
Gastrointestinal: Salivary, esophageal mucosal, gastric secretions and secretions at various levels of the intestine are inhibited, motility decreases, and sphincter tone increases. There is a slight antispasmodic effect on the bile ducts and a delay in gallbladder emptying, even in the presence of fatty foods.
Urinary tract: Dilates the smooth muscle of the bladder and decreases the contractility of the urethra.
Uterus: Produces only slight effects on uterine motility, in a gravid uterus or a number.
Skin and Appearances: Reduces natural perspiration by decreasing the secretion of the sweat glands. These effects can generate hyperthermia.
Sense organs: It can cause mydriasis and cycloplegia.
Clinical pharmacology: It is broad and applies to various clinical specialties. REDOTEX® is interested in its property of slowing the heart rate and inhibiting reflexes of salivary and gastric secretion, associated with physiological hunger, in the presence or absence of food, during periods of wakefulness. This occurs at low doses, decreasing salivation that initiates the physiological cascade of tract secretions on the one hand and gastric M1 inhibition on the other.
Aloin: Cathartic agent whose active ingredient is anthraquinone, light laxative well tolerated.
Diazepam: The obese is a patient who frequently presents with anxiety. Anxiety disorders that can be treated with anxiolytics include generalized anxiety disorder, panic disorder with and without agoraphobia, specific phobic disorders, acute stress disorder, obsessive-compulsive disorder, and post-traumatic stress disorder. Diazepam carries out its anxiolytic activity through an increase in
GABA-ergic activity at all levels of the CNS, by stimulating the GABA-A receptor complex that induces a decrease in excitatory neural reactivity. Diazepam increases coronary blood flow possibly by increasing adenosine concentration. Anxiolytic doses of diazepam are approximately 5 mg, usual therapeutic doses are in the range of 5-40 mg daily, and sedation and drowsiness are the most frequent acute adverse effects of benzodiazepines that normally reach their greatest benefits after 6 week latency. People can develop tolerance to extremely high doses (up to 1,000 to 1,500 mg per day) of diazepam. Tolerance to the sedative-hypnotic effects may develop in 2 to 3 weeks, however, the anti-anxiety effects persist. In view of the controversy surrounding long-term medication use, routine discontinuation after 6 months to a year is appropriate; patients should discontinue medication for at least one month before restarting treatment to allow adequate time for adjustment after discontinuation.
Many patients and their physicians maintain that the anti-anxiety benefits persist long after tolerance to the sedative effects has occurred, yet these patients continue to take the drug for years as directed by their physician, without increasing the dose, with sustained efficacy over time. So keep taking the benzodiazepine. Diazepam has been described as a benzodiazepine receptor agonist, which has been involved in the dysfunction of homeostasis control mechanisms. It has been shown in experimental animals that the limitation of this drug reduces weight gain, also reducing the concentration of insulin in obese specimens.
Adverse effects: Benzodiazepines can cause lightheadedness, lassitude, increased reaction time, motor incoordination, confusion, anterograde amnesia, weakness, headache, blurred vision, vertigo, nausea, arthralgia, and incontinence. They are contraindicated in patients with sleep apnea.
Pharmacological interactions: They can induce digoxin toxicity by reducing its excretion. Long-acting benzodiazepines are vulnerable to medications that inhibit liver enzymes and to cimetidine. Estrogens, tobacco, methylxanthine derivatives tend to reduce benzodiazepine levels.
It has recently been described that benzodiazepines are CCK agonists, which constitutes a second satiogenic action.
Interaction Rationale:
D-Norpseudoephedrine hydrochloride: By acting at the level of the hypothalamic centers, it raises the hunger threshold and maintains a feeling of satiety, while decreasing “psychic hunger”, without associated central stimulation, or tolerance or dependence phenomena. Its peripheral thermogenic effect is also useful.
Triiodothyronine: Maintains the relative T3 deficit that may be present in obese patients undergoing weight loss, increases fat catabolism without altering thyroid function towards pathological forms, and uncouples the respiratory chain, increasing energy loss in the form of heat.
Hypothyroidism can cause weight gain. Thus, obese patients with Acanthosis nigricans, leg cramps, anemia and/or hyperlipidemia may have thyroid disease.
Since the beginning of the 20th century, t3 has been used within the general scheme of treatment for obesity. Heckel in 1911 accepted thyroid therapy, conditional on the dose. In 1961 Goldbereg raised the possibility of euthyroid hypometabolism, which Gordon called metabolic obesity. In France, the obese person with hypothyroidism was called Klotz’s Lazy Thyroid. For Cormillot, in cases of hypothyroidism with obesity or when weight loss stops, or when oxygen consumption decreases, thyroid hormone therapy was indicated and it was observed that with high doses of T3, up to 200-250 μg, obese patients show no signs of thyrotoxicosis.
Today it is known that obesity is a low-intensity inflammatory disease, and that adipocytes secrete cytokines, including Tumor Necrosis Factor (TNF) and interleukin 1 (IL1). TNF, IL-1, and interferon-gamma can make thyroid cells more susceptible to apoptosis mediated by death receptors such as Fas; thus, elevated levels of cytokines intensify thyroid autoimmune disease. That is why the substitution of T3 levels, 75 μg in prolonged release presentation, allows a better control of the entity, without the presence of factitious thyrotoxicosis.
Atropine: At this dose, heart rate decreases, counteracting the cardio-accelerator effect of sympathomimetics. Decreases gastric and salivary secretions, inhibiting hunger reflexes and the physiological cascade of the gastrointestinal tract.
Aloin: Counteracts the effects of decreased intestinal motility induced by atropine and constipation that is usually present in the obese.
Diazepam: Due to its anxiolytic action, it keeps the patient without anguish, reducing bulimic neurosis and consumption automatisms, favoring adherence to the diet because it does not cause anxiety and achieving successful treatment more easily and collaborates with its satiogenic action as a CCK agonist.
Due to additive synergy, the components of the formula show efficacy for the optimal treatment of obesity, with few or rare adverse effects. Also without risk of misuse, abuse or tolerance. With the presentation of dialicels, a prolonged release is maintained for 8 hours, without “absorption peaks” or “elimination valleys” reaching therapeutic concentrations for 10 to 12 hours in the initial administration, contributing to adherence to treatment. A double-blind, placebo-controlled, comparative study of the efficacy and safety of REDOTEX® in the Mexican population demonstrated the efficacy and safety of the drug in patients treated for 6 months, achieving weight loss of 14.9% of their initial weight.
CONTRAINDICATIONS: REDOTEX® should not be administered to patients with obesity of endogenous origin, as well as those with severe neurological, psychiatric or personality disorders. Hyperthyroidism, heart disease, high blood pressure, diabetes, liver and/or kidney failure, glaucoma. Anorexia, chronic insomnia, psychopathic personality, suicidal or homicidal tendencies. Glaucoma. Prostatic hypertrophy or any obstructive disease of the urinary tract or gastrointestinal tract. During pregnancy or lactation. Concomitantly with MAOIs or with other adrenergic or β-blockers.
RESTRICTIONS OF USE DURING PREGNANCY AND LACTATION: They should not be administered to women during pregnancy or lactation. Effective means of contraception should be recommended during treatment in sexually active women of childbearing age.
SECONDARY AND ADVERSE REACTIONS: These correspond to those described for sympathomimetics and are expected according to their mechanism of action and are usually well tolerated for a few days if treatment is continued: nervousness, insomnia, excitement, fatigue, mydriasis, photophobia, cyclopegia, palpitations, tachycardia, dry mouth and mucous membranes, flushing, nausea, vomiting, constipation or diarrhea, erythema, dysuria, urinary retention, otherwise the drug should be discontinued.
Post-Marketing Experience: Adverse actions reported from post-marketing experience include the following:
• Gastrointestinal disorders: dry mouth, constipation and nausea.
• Metabolism and nutrition disorders: Polydipsia, thirst and early satiety.
• Psychiatric disorders: Anxiety, nervousness, drowsiness, irritability and insomnia.
• Central nervous system disorders: Headache, dizziness, fine tremor.
• General disorders and administration site conditions: Asthenia and fatigue.
• Cardiac disorders: Tachycardia and palpitations.
• Musculoskeletal and connective tissue disorders: Chills.
• Skin and subcutaneous tissue disorders: Alopecia.
• Vascular disorders: Hypotension.
• Reproductive system and breast disorders: Erectile dysfunction and menstrual disorders.
DRUG INTERACTIONS AND OTHER GENDER:
Concomitant administration of D-norpseudoephedrine with:
• Monoamine oxidase inhibitors (MAOI): It is contraindicated, since severe hypertensive crises may occur; In addition, the subsequent administration of an MAOI must be done at least fourteen days after its interruption.
• β Blockers: They can increase the activity of α adrenergic receptors or amplify the adverse effects associated with their stimulation.
• Digitalis: They can cause heart rhythm disorders.
Concomitant administration of L-triiodothyronine with:
• Oral anticoagulants: Their activity may be enhanced. Bleeding, coagulation, and prothrombin times should be monitored and doses adjusted.
• Insulin or oral hypoglycemic agents: Their requirements are increased. Blood glucose should be monitored and doses adjusted.
• Cholestyramine: Binds to T3 and T4 in the intestine, thus reducing its absorption. In this way, they must be administered separated from food for 4 to 5 hours.
• Estrogens and oral contraceptives: In cases of non-functional thyroid, T3 requirements are increased.
• Tricyclic antidepressants: The effects of T3 and AT are enhanced. The presence of cardiac arrhythmias should be monitored.
• Digitalis: T3 can enhance their toxic effects; In addition to increasing your requirements.
• Ketamine: Hypertension and tachycardia may occur.
Concomitant administration of atropine with:
• Tricyclic antidepressants: Adds central and peripheral anticholinergic effects. Cardiac dysrhythmias, urinary retention and constipation may occur.
• Antihistamines, barbiturates and phenothiazines: their effects are enhanced.
• Reserpine or neostigmine: Their effects are attenuated or nullified.
• Aloin does not present interactions of clinical interest.
Concomitant administration of diazepam with:
• Cimetidine, disulfiram, erythromycin, isoniazid, ketoconazole, metoprolol, oral hormonal contraceptives, propoxyphene, propranolol and valproic acid: It can cause a reduction in metabolism, thus prolonging its half-life.
• Contact antacids: They can inhibit the speed of its absorption, but not its plasma concentration.
• CNS depressants, such as tranquilizer neuroleptics, antidepressants, hypnotics, anticonvulsants, narcotic analgesics and anesthetics, as well as antihistamines and barbiturates: They can enhance their action.
• In general: Alcohol intake should be avoided during treatment.
CHANGES IN THE RESULTS OF LABORATORY TESTS: During treatment, TSH and T4 levels are reduced, but the euthyroid state is maintained.
DOSAGE AND ROUTE OF ADMINISTRATION:
Dosage: One capsule daily on an empty stomach, for periods of up to six months.
Administration way: Oral.
MANIFESTATIONS AND MANAGEMENT OF OVERDOSAGE OR ACCIDENTAL INGESTION: There are no known cases of over dosage by REDOTEX® reported (by usual prescribers) in any way, in the case of an over dosage, this would consist of an exaggeration of both the sympathomimetic effects of D- norpseudoephedrine, like atropine anticholinergics. These can be countered by general and specific measures. Depending on the time of ingestion, a gastric lavage may be indicated in a conscious patient, as well as accommodating him in a dark and quiet place. Maintenance of patent airways and vascular pathways, control and monitoring of vital signs. Hemodialysis may be indicated.
The use of neostigmine-type anticholinesteracics can counteract and abolish anticholinergic intoxication. The use of sympatholytics can counteract or abolish sympathetic intoxication. The use of benzodiazepine-type anxiolytics is indicated to avoid over-stimulation of the CNS.
Symptoms: These are dose dependent associated with:
• D-norpseudoephedrine: Headache, nervousness, insomnia, delusional blufee, tachycardia, and rise or fall in blood pressure.
• L-Triiodothyronine: Headache, irritability, nervousness, diaphoresis, tachycardia and meteorism.
• Atropine: Restlessness, tremor, seizures, coma, delirium, dry mucous membranes, cycloplegia, photophobia, tachycardia, dysrhythmias, colic-type pain, constipation, urinary retention, and hyperthermia.
• Aloin: Diarrhea.
PRESENTATIONS:
Box with bottle with 30 capsules.
Box with 30 capsules.
Buy fat burners online USA.
Related products
Megabol 200mg/ml 10ml – Medical Pharma
$99.00Add to cartMetandienone (pINN); Metandienon; Metandienona; Métandiénone; Metandienoni; Metandienonum; Methandrostenolone; NSC-42722.17β-Hydroxy-17α-methylandrosta-1,4 dien-3-one.
C20H28O2 = 300.4.
CAS — 72-63-9.
ATC — A14AA03; D11AE01.
ATC Vet — QA14AA03; QD11AE01.NSC-9166; Propionato de testosterona; Testosteron Propiyonat; Testostérone, propionate de; Testosteroni propionas; Testosteronipropionaatti; Testosteronopropionatas; Testosteronpropionat; Testosteron-propionát; Testosteronu propionian; Tesztoszteronpropionát. 3-Oxoandrost-4-en-17β-yl propionate; 17β-Hydroxyandrost-4-en-3-one propionate.
Provir (Mesterolone) 50mg/tab 100 tabs – Medical Pharma
$93.00Add to cartPharmacologic Category
Androgen.
Dosing: Adult
50mg every days for duration of 4-8 weeks.
Dosing: Geriatric
Refer to adult dosing.
Dosing: Pediatric
No information in pediatric population available.
Dosing: Renal impairment
No dosage adjustment provided in manufacturer’s labeling; use with caution due to propensity to cause edema.
Dosing: Hepatic impairment
No dosage adjustment provided in manufacturer’s labeling; use with caution.
Decadurabolin “Decabol” 300mg/ml 10 ml – Medical Pharma
$93.00Add to cartDecanoato de nandrolona; Nandrolon-dekanoát; Nandrolone, décanoate de; Nandroloni decanoas; Nandrolonu dekanonian; Nortestosterone Decanoate; Nortestosterone Decylate. 3-Oxoestr-4-en-17β-yl decanoate; 17β-Hydroxyestr-4-en-3-one decanoate. Нандролона Деканоат.
C28H44O3 = 428.6.
CAS — 360-70-3.
ATC — A14AB01; S01XA11.
ATC Vet — QA14AB01; QS01XA11.Pharmacopoeias. In Eur.(see p.vii) and US.
Tri Trenabol 150mg/ml 10 ml Trenbolone Blend – Medical Pharma
$93.00Add to cartTrenbolone Acetate
Trenbolone Acetate; Acetato de trenbolona; RU-1697; Trenbolone, Acétate de; Trenboloni Acetas; Trienbolone Acetate. 17β-Hydroxyestra-4,9,11-trien-3-one acetate.
Pay with WISE APP or Remitly
Pay with WISE App or Remitly
Fast money transfers from USA for fast delivery of steroids
Secure delivery in USA
100% reliable shipping in USA
24x7 Support
Online 24 hours
Low cost delivery
Great shipping prices in USA
BULK ORDER DISCOUNT
If you are a reseller in the USA you can get a special DISCOUNT, we can give you up to 50% or more on bulk orders. If you want to make a bulk order, we can negociate for orders of over USD$4,000, contact us by email.
Steroids info